Antibiotics are not the perfect fix to every illness
November 16, 2021

Learn when antibiotics heal, and when overuse causes problems
No one wants to be sick and, when you or a loved one aren’t well, it is natural to turn to doctors, hoping they’ll prescribe the medicine that will help you and yours feel better. Antibiotics are often requested by patients desperate to hasten their healing—but there are cases in which antibiotics are unnecessary and can do more harm than good.
US Antibiotic Awareness Week (USAAW) is November 18 – 24. This one-week observance takes place each year to help healthcare providers educate their patients on the appropriate use of antibiotics and how to avoid antibiotic resistance.
According to the CDC, at least 28% of antibiotics prescribed in U.S. outpatient settings are unnecessary. It is important to know when antibiotics are appropriate and how to feel better when they aren’t. Check out the five most frequently asked questions below to learn more.
I feel terrible. Why won’t my doctor prescribe antibiotics?
It’s understandable to want to feel better when you’re ill, but antibiotics aren’t always the answer. “Patients often expect antibiotics for their illnesses based on prior experiences with the health care system in which their doctor prescribed an unnecessary antibiotic in order to “do something” and or meet the patient’s expectations,” said Texas MedClinic Chief Operating Officer and practicing physician Dr. David Gude. “In many cases, antibiotics will not make them better faster and can do more harm than good.”
Many of the illnesses we contract, including colds, the flu, and COVID-19, are caused by viruses and cannot be treated with antibiotics. If you are suffering from a viral infection, antibiotics will not make you feel better. Most viruses go away on their own within a week or two.
There are antiviral agents like Tamiflu that treat the influenza virus. There are two companies currently seeking FDA Emergency-Use-Authorization for medications that treat COVID-19, which in clinical trials are showing strong results.
When should I take antibiotics?
Antibiotics are prescribed to treat certain bacterial infections, like:
- Strep throat
- Urinary tract infection (UTI)
- Some sinus and ear infections
- Skin infections such as impetigo and cellulitis
- Whooping cough
The CDC has created the following chart to help you determine if your illness could require antibiotics.
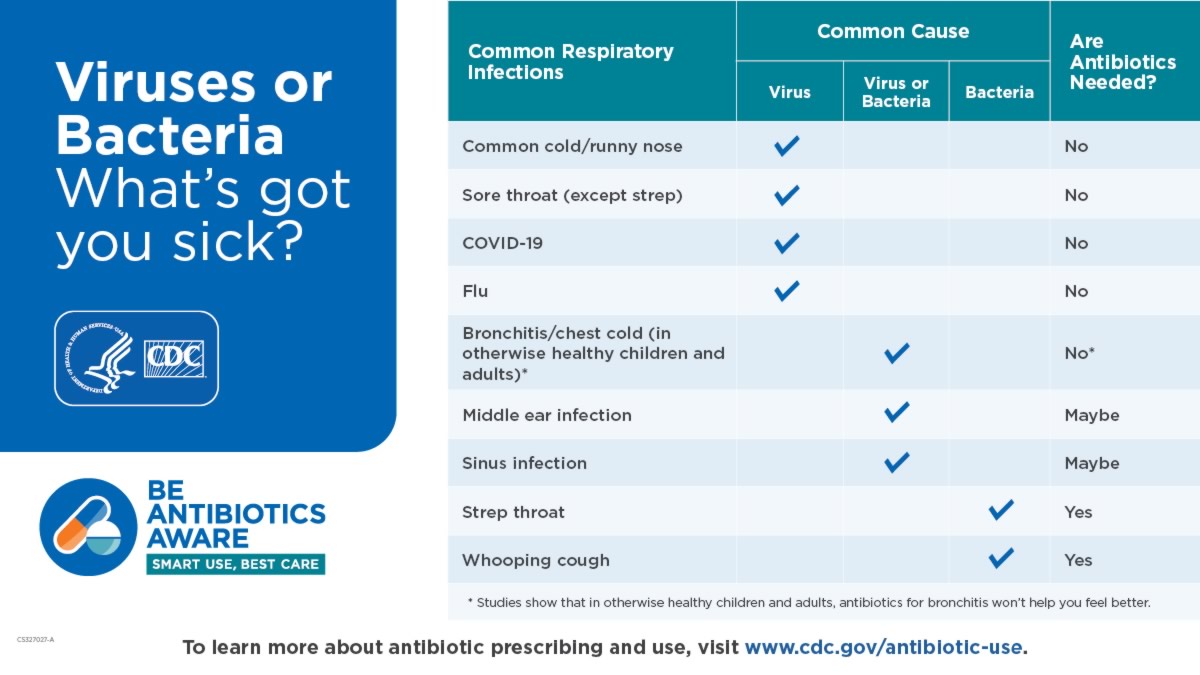
What’s wrong with taking antibiotics when they aren’t needed? Isn’t it better to be safe than sorry?
No. Antibiotics should only be used in cases where the benefit of taking antibiotics outweighs the risk of side effects and antibiotic resistance.
Antibiotic resistance means that the bacteria causing the illness has developed the ability to defeat the antibiotic that was designed to kill it. When antibiotics become ineffective against bacteria, doctors can no longer use that drug to treat the infection. Using antibiotics when they are not necessary is a major contributor to this phenomenon.
Would my doctor prescribe antibiotics even if they are medically unnecessary?
The sad truth is, maybe. Unfortunately, some doctors follow the path of least resistance, finding it easier to prescribe antibiotics to an expectant patient than explain why antibiotics won’t help.
This is why it is critically important that you find a clinic or doctor where you feel confident in the care provided and trust the recommendations made by them.
What can I do to feel better if I am suffering from a viral infection?
Here are some tips that can help you feel better:
- Stay home and get as much rest as possible. Avoid close contact with others living in your home to reduce the chance of spreading the virus to them.
- Drink plenty of water and other clear liquids to avoid dehydration.
- Over-the-counter medicines like ibuprofen (Advil), acetaminophen (Tylenol), cough medicines, and decongestants can help alleviate symptoms like body aches, sore throat, cough, and congestion. Always read labels carefully and follow dosing instructions.





